Sierra Leone has denied report by the World Health Organization (WHO) that it has recorded cases of Monkeypox this year.
In a statement on May 31, the WHO Africa regional office listed Sierra Leone among seven countries it said had recorded cumulative cases of 1, 400. The other countries are Liberia, Nigeria, Cameroon, Central African Republic, the Democratic Republic of the Congo and the Republic of the Congo.
According to the statement, 1, 392 of the reported cases were suspected, while 44 had been confirmed. It adds that the case count is for the year up until mid-May.
But a spokesman for the Ministry of Health said there has been no report of suspected Monkeypox outbreak in the country this year. Harold Thomas, Communications Lead at the Directorate of Health Security and Emergencies (DHSE), said while Sierra Leone had recorded cases of the viral disease in the past, there has been no reported case this year.
“It’s totally wrong. You know whenever we record cases [of emergency health issues] we come public about it,” Thomas told ManoReporters, when asked why would WHO list Sierra Leone among countries with cases.
The WHO Country office did not respond to a request for comment. But a source told ManoReporters that the local office didn’t report any such case to the regional office.
Monkeypox is a viral disease that can spread from animals to humans but can also spread between people through close contact with an infected person.
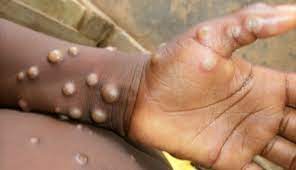
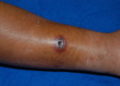
Symptoms typically include skin rash or lesions, fever, intense headache, muscle aches, back pain, low energy and swollen lymph nodes. In many patients, the symptoms clear up on their own between two to four weeks, but severe cases and even death can occur.
The case fatality ratio for monkeypox is estimated at around 3-6%, according to WHO.
Sierra Leone, which is considered as endemic to Monkeypox, is one of the first countries in Africa to record cases of the virus which falls under the genus orthopoxviruses.
Monkeypox was first isolated in laboratory monkeys in Denmark, in 1958. The first human case was detected in the Democratic Republic of Congo in 1970.
For decades only a few cases were reported sporadically across the world. In 2017, there was a sudden spike, with more than 2,800 suspected cases reported in five countries. This surge continued, peaking in 2020 with more than 6,300 suspected cases, with the DRC accounting for 95% of the total.
The numbers then dropped last year to around 3,200 suspected cases.
Described as a tropical zoonosis, Monkeypox is known to be mostly present in West and Central Africa. The West African strain is said to have far less fatality rate, at 4 percent, compared to the central African strain, according to the United States Centers for Disease Control.
Sierra Leone recorded its first human case in 1970. And in 2019, after 44 years, it reported another case.
A report by the US-based National Library of Medicine cites a 2007 survey for orthopoxvirus antibodies that generated evidence to suggest ongoing circulation of orthopoxviruses among populations near the eastern Kenema district.
The current global monkeypox outbreak began after a case was reported in the UK on May 6, 2022. The patient reportedly fell ill after returning from travels in Nigeria. But reports later suggest that cases were already spreading in Europe.
As of June 14, WHO data show that more than 1,600 confirmed cases and almost 1,500 suspected cases have been reported, across 39 countries. These figures include 32 non-endemic or newly-affected nations.
WHO’s panel of experts is scheduled to meet on June 23 to assess whether the continuing outbreak represents a Public Health Emergency of International Concern, the highest level of global alert, which currently applies only to the COVID-19 pandemic and polio.
The WHO Africa office said that while the virus has not spread to non-endemic countries in the region, it has been expanding its geographic reach in recent years.
There is only one vaccine specifically made for Monkeypox, called Imvanex. But it is only approved for use on people 18 years and above and it is not widely available.
Some vaccines for smallpox are also said to be effective against monkeypox.
Dr Matshidiso Moeti, WHO Regional Director for Africa,
called for fair distribution of response effort between Africa and Europe where the international response is currently focused.
“We must avoid having two different responses to monkeypox – one for Western countries which are only now experiencing significant transmission and another for Africa,” she said, adding: “We must work together and have joined-up global actions which include Africa’s experience, expertise and needs. This is the only way to ensure we reinforce surveillance and better understand the evolution of the disease, while scaling up readiness and response to curb any further spread.”
According to Dr Moeti, it is critical that the continent has equal access to effective monkeypox vaccines and to ensure that vaccine doses reach every community in need.
“While parts of the continent might have built up some immunity against the disease, there are populations that are particularly vulnerable such as health workers and contacts of cases,” she said.