By MSF
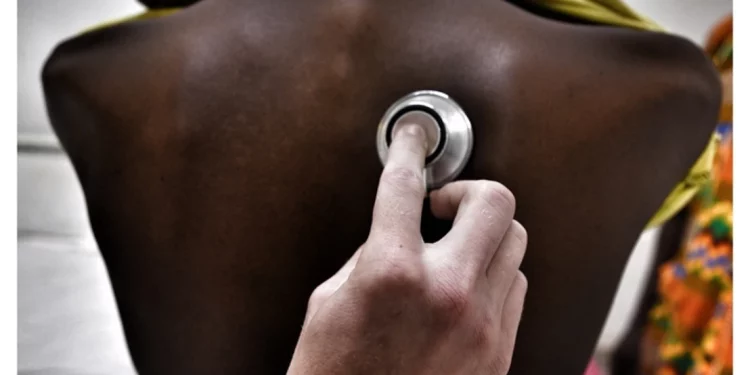
Sierra Leone has a high burden of drug-sensitive tuberculosis, an estimated 23,000 TB patients each year with about 640 multidrug-resistant Tuberculosis (MDR-TB) new patients each year. Less than half of the Multidrug-Resistant tuberculosis (MDR-TB) cases in the country are diagnosed and treated, and only 14 per cent of health facilities in Sierra Leone have TB services.
TB patients’ access to diagnosis and care is hampered by many challenges, especially in rural areas. Long distances, bad roads and high costs of transportation are some of the obstacles preventing patients from seeking care.
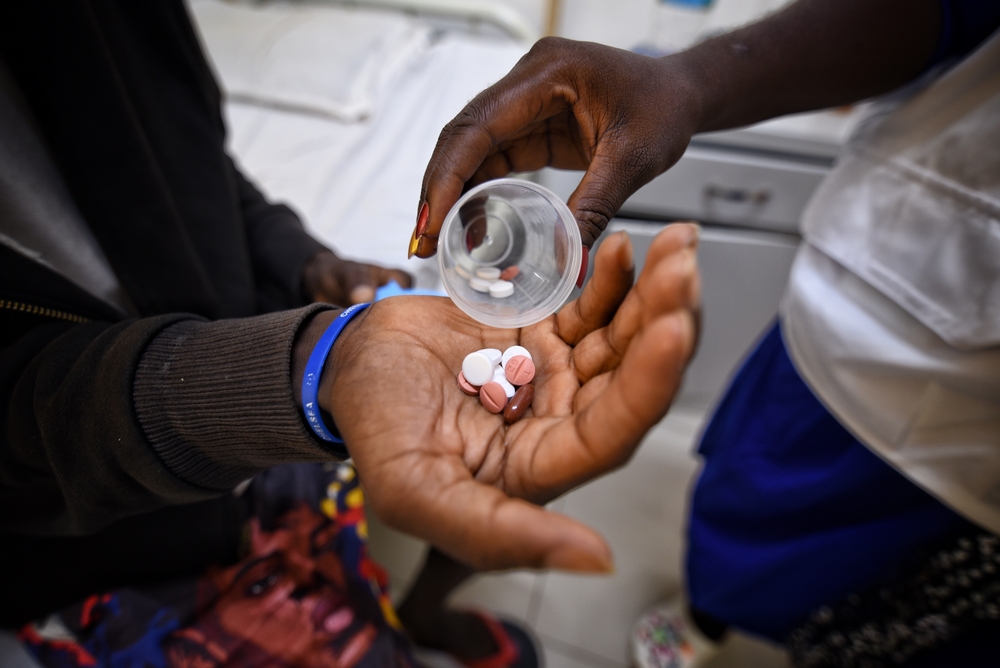
Once diagnosed, treatment for TB patients can be long and difficult, often involving harsh drugs and debilitating side effects, especially for those with multi-drug resistant tuberculosis (MDR-TB), who often face long periods of hospitalisation. These factors make it difficult for many patients to stick to treatment.
Outpatient, holistic and patient-centred care
Working with the National Leprosy and Tuberculosis Control Program (NLTCP) of Sierra Leone’s Ministry of Health and Sanitation (MoHS), MSF has introduced strategies to simplify the treatment, make it more tolerable, and bring it closer to patients. MSF is supporting Sierra Leone’s first decentralised DR-TB centre in Makeni Regional Hospital, which opened in 2020. The hospital provides outpatient care to patients coming from a wide catchment area in the district, using short, oral DR-TB regimens.
“The outpatient care model allows patients with drug-resistant TB to take their medication at home,” says Omer A. Abdalla, MSF Country Director in Sierra Leone. “While the hospital also has inpatient capacity, patients can now stay in their communities.”
Patients without any health concerns that need close observation are started on treatment in their homes and continue treatment there. A treatment buddy, identified by the patient, encourages the patient to continue taking their medication. The patient and treatment buddy come to the hospital each month to collect drugs and to do follow up check-ups.
To improve treatment adherence, counselling and mental health support are provided to patients. Measures to improve the ability for people to stick to treatment, such as transportation allowances and nutritional support for patients and caregivers, also play a key role in making it easier for patients to continue with their treatment.
Better access to diagnosis
MSF also supports 12 directly observed therapy (DOT) sites in Bombali district. To increase access to diagnosis, MSF has implemented a sputum transportation system in Bombali district. Sputum samples are collected from basic healthcare centres, such as clinics, and DOT sites by motorbike and brought to Makeni hospital, where GeneXpert testing machines can diagnose TB.
Raising awareness in the community
To raise awareness on tuberculosis, address knowledge gaps and stigma, MSF carries out health promotion activities in the community. One of the key activities is engagement with traditional healers. They are trusted members of the community and in a country with few trained medical professionals, often the first point of contact for people when they are sick.
“MSF has provided training to 500 traditional healers in Bombali district to enable them to recognise symptoms of tuberculosis, and to refer suspect patients faster to health facilities,’ says Osman Bangura, MSF Health Promotion Supervisor.
Part of MSF’s efforts and holistic approach is also to improve access to treatment for TB patients in difficult living and hygiene conditions, such as prisons.
“In Makeni Correctional Centre, MSF constructed a TB site for consultations and treatment of TB for inmates and staff,” says Mohammed Moqbel, MSF Project Coordinator in Sierra Leone. “A team goes once a week to screen patients suspected of having TB and provide treatment in the centre.”
Since the start of the DR-TB programme in Makeni in early 2020, a total of 98 patients were started on treatment, with 44 patients being enrolled in the modified short (9-12 months) oral regimen.